Medicaid change means many have lost dental, vision benefits
Published 7:39 am Wednesday, July 4, 2018
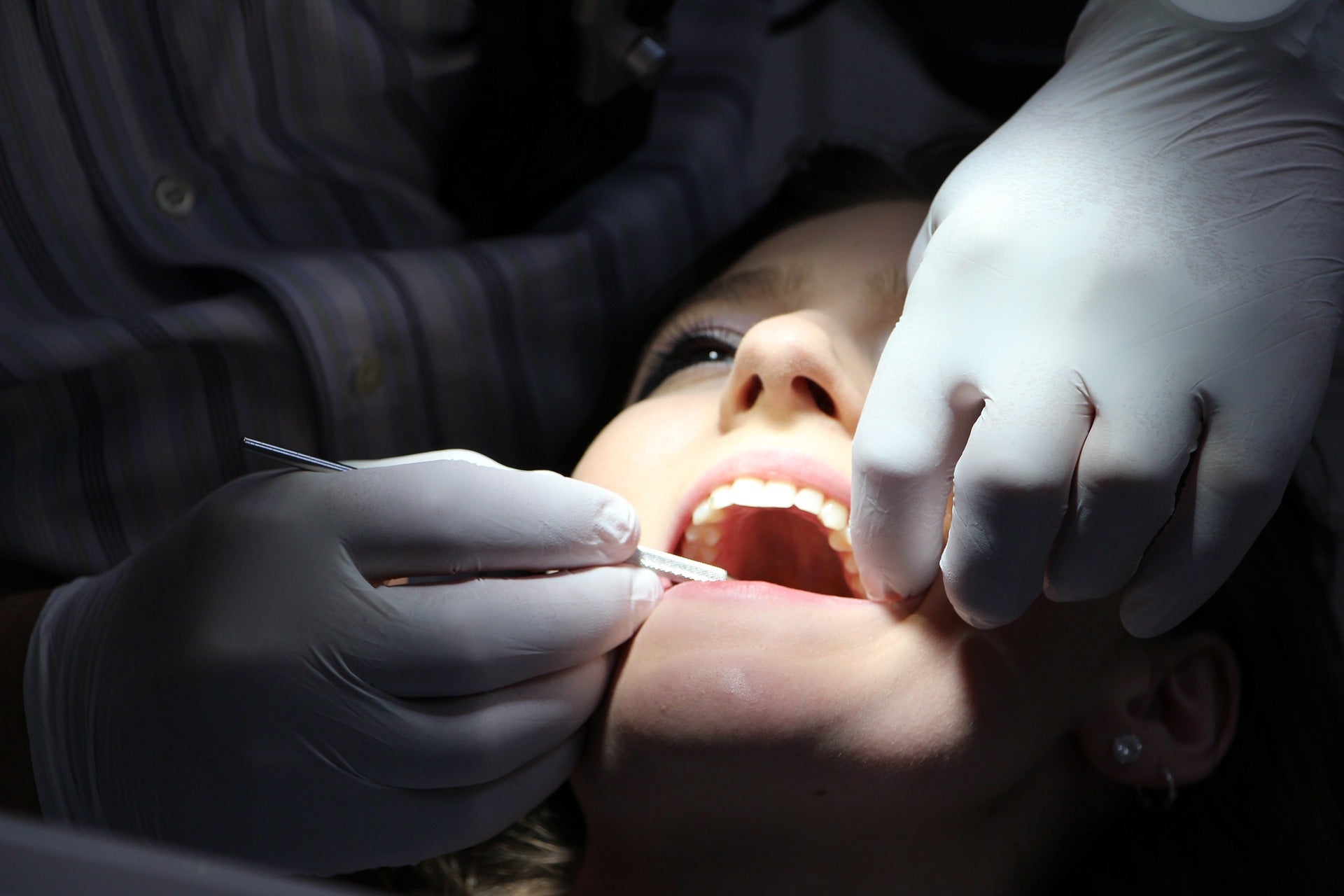
- Public domain
Although he’s director of the Boyle County Health Department, Brent Blevins — as well as many, many others — wasn’t made aware of a huge change in the state’s Medicare program until he saw headlines over the weekend.
On Friday, a court ruling blocked Gov. Matt Bevin’s Medicaid proposal. It was a huge setback for the governor, as well as the Trump administration, in attempts to change the law in order to allow states to impose Medicaid work requirements more broadly.
Last weekend, Gov. Bevin’s administration canceled dental and vision benefits affecting almost 500,000 Kentuckians enrolled in the state’s Medicaid expansion.
Boyle Health Department Director Blevins says unfortunately, he doesn’t know much more than the public does at this time. But what he does know is when a drastic change like this is made, “All of a sudden you have a whole group of people who go from some type of coverage to no coverage.”
U.S. District Court Judge James Boasberg ruled the Trump administration didn’t consider coverage losses that would result in the work requirements, saying it goes against the program’s aim of providing health insurance. It wasn’t long after that ruling the state Cabinet for Health and Family Services began posting a public notice on its website that vision and dental services would be no longer be covered by members’ My Rewards accounts.
“If we don’t have a good program or option for those people to pick up quickly, you’ll have people going without coverage for extensive lengths of time,” Blevins says. “And if they need additional funding to pick up the coverage they had, how will that happen?”
At almost half a million Kentuckians, “That’s a lot of people,” he said. “Dental and vision are one of those vital services we should all have. Dental hygiene and health is incredibly important to overall health.”
According to Kentuckyhealthfacts.org, Medicaid enrollment in Boyle County totals 5,709 people, equal to 20 percent of the county’s population.
Bevin’s Kentucky HEALTH program, also known as the 1115 Medicaid waiver, was due to go into effect July 1, but did not because of the ruling that came as a result of a lawsuit filed by Medicaid recipients, asserting the waiver was illegal and would result in many losing benefits.
Bevin had already filed an executive order for his administration to end Medicaid expansion if any part of the waiver was upended due to a legal challenge. As of now, the issue is not fully resolved; the decision can be appealed.
“It sounds to me like the state is blaming the benefits reduction on the judge’s ruling,” says Emily Beauregard, executive director for Kentucky Voices for Health, an advocacy group with offices in Frankfort and Louisville. But Beauregard says as far as she can tell by reading Medicaid rules, it’s completely voluntary.
“Kentucky does not need to reduce Medicaid benefits to reduce the numbers. The way they’ve gone about reducing these benefits is not by following the federal rules.”
She says they skipped a number of important steps required. Those steps include the approval of Centers for Medicare & Medicaid Services’ (CMS) to reduce services; filing of a revised state regulation; holding a public comment period; and informing affected Medicaid members and providers.
“The result is we’ve heard from providers, as soon as Monday morning, because they don’t know who’s covered.
Most providers are confused” and don’t know if they’ll get reimbursed if they provide the service, Beauregard says. “I know the state told one provider he can go on and see the patients, and if the state doesn’t pay, then they can bill the patient. Well, they probably can’t pay; that’s why they have Medicaid. That’s the issue we’re having now — they’re canceling services on members.”
This will affect about half a million people, she says — one in 10 Kentuckians. Beauregard says it’s been nothing short of massive chaos and confusion.
“As far as we know, the decision was made Friday night. And there was a Facebook post telling people if they were on the expanded Medicaid, they were losing their dental and vision benefits,” Beauregard says. “… So over the weekend, how many people you think figured out what happened and who was affected? Come Monday, people who had scheduled their appointments weeks, sometimes months ago went in to get their services, and providers were just finding out something had changed and didn’t know what to do.”
That resulted in many members getting turned away. Beauregard says some providers decided to eat the costs if they don’t get reimbursed, but not all practices can do that.
Beauregard says part of the confusion stems from the fact that since the judge blocked Bevin’s Medicaid waiver, and the My Rewards account was a part of the waiver, the state said it had already made changes so that expansion members could earn their vision and dental benefits through the new system.
“But the changes hadn’t been made, and it hadn’t been approved through CMS, and the state didn’t file anything.”
What will happen is people won’t get the care they need, which goes against the whole purpose of having Medicaid, Beauregard says.
“It’s our health care safety net. It’s supposed to be there for people when they need it.”
Beauregard says the move will lead to a trickle down effect, causing more and more people to turn to emergency rooms due to conditions they’ve left untreated.
“For people with dental pain, they will end up in the ER and be treated with an antibiotic and pain medication. Dental pain is a gateway to opioid addiction — if you’re untreated, it’s the only way to treat the pain,” she says.
Beauregard found out from research that non-emergency transportation coverage was also eliminated in the move. People on Medicaid were previously able to get transportation for medical treatment covered; now, Kentucky’s Medicare expansion no longer offers that coverage.
“If you think about ways we can eliminate barriers to health care, this is the complete opposite. This is putting up more barriers,” she says.
Blevins and Beauregard both say the best move for people concerned by the change is to contact their legislators. Beauregard says those directly affected — members and providers — can appeal the change, as well.
“They can contact their Medicare managed care organization and talk to someone at their local legal aid program, let them know they’ve been denied services,” she says.
Blevins says contacting legislators personally is important. He says it’s good for lawmakers to hear directly from individuals.
“Advocacy groups are important, but individuals need to make that contact,” he says. “If enough of them make it, maybe they can go further to figure it out. If it goes away altogether, it would be tremendously concerning.”
Blevins says it will make quite a difference in Danville if 1,000, or even 500 people lose their ability to get affordable dental and vision care.
“That would be a significant issue in our community,” he says.
Beauregard says so far, the state hasn’t offered any type of electronic way for people to file comments about the move during the public comment period; only a snail mail address.
The notice was posted Saturday; people have 30 days from then to comment. Kentucky Voices for Health will be collecting comments from members and providers who are directly affected by the change, printing them out and sending them to the state. A survey is on the organization’s website (kyvoices4health.org) and Facebook page.
“The administration has to be held accountable to follow the rules of Medicaid. They haven’t done this,” Beauregard says. “Secondly, people can contact their legislators and tell them they want dental and vision benefits mandatory for all members.”
Some lawmakers have already begun work on a bill to do just that, she says.
All the organization has been doing for the past two years has been focusing on the governor’s Medicaid reform effort, Beauregard says.
“I’d love to be able to work on things like quality of care, more patient-centered care, but right now we have to focus on people actually not able to get care. We’re having to focus on protecting people’s basic access to care.”
SO YOU KNOW
For Medicaid members and providers affected by the benefits change, comments will be accepted at kyvoiceforhealth.org, and the organization’s Facebook page, kyvoices4health. Members may also log onto benefind.ky.gov to check their benefits status.




